Understanding the early signs of psoriatic arthritis is crucial for prompt diagnosis and treatment, especially when it comes to the feet. Affecting the toes and ankles, psoriatic arthritis can significantly impact mobility and quality of life. However, diagnosing the condition can be complicated due to its subtle initial symptoms. This article provides a detailed look at early stage psoriatic arthritis in feet, supported by pictures to help you identify the condition.
Visual Signs of Psoriatic Arthritis in Feet
Redness and Swelling
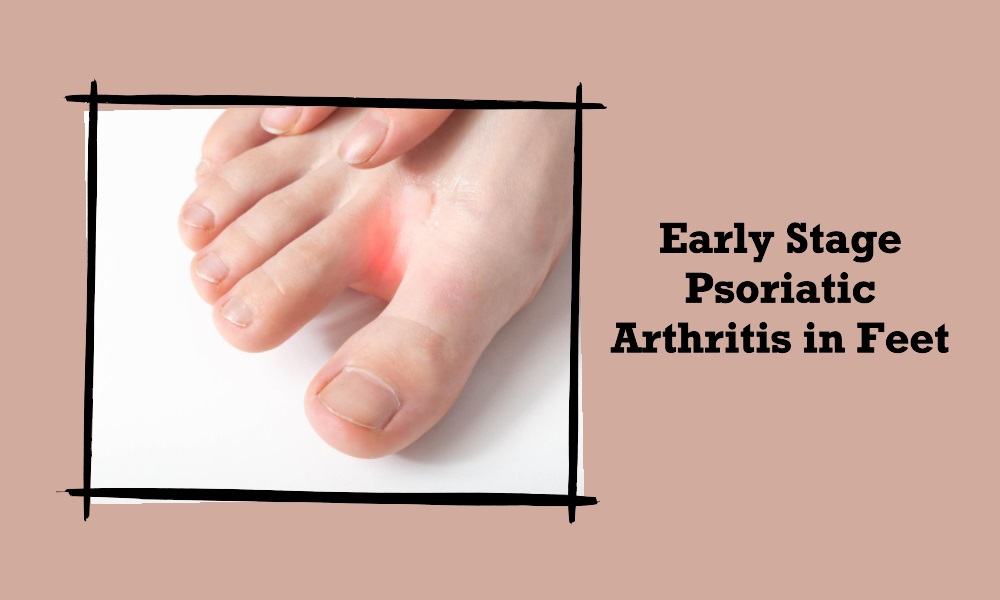
Picture Description: Mild redness and swelling around the joints of the toes or ankle.
Initial symptoms often involve mild redness and swelling around the toe and ankle joints. Unlike normal inflammation, the redness often extends beyond the affected joint.
Nail Changes
Picture Description: Yellowing or pitting (small dents) in the toenails.
Psoriatic arthritis often manifests in the nails as yellowing or pitting, which are small dents in the surface of the nails.
Skin Plaques
Picture Description: Silver, scaly patches on the skin around the feet or ankles.
In many cases, the characteristic psoriasis skin plaques accompany joint symptoms, manifesting as silver, scaly patches around the feet and ankles.
Symptoms Accompanying Visual Signs
Pain and Discomfort
While redness and swelling are visible signs, they are often accompanied by varying degrees of pain, particularly during movement or after periods of inactivity.
Reduced Range of Motion
The inflamed joints often limit the range of motion in the feet, making it challenging to walk or perform activities that require foot flexibility.
Stiffness
Joint stiffness is a common issue, especially in the mornings or after long periods of immobility, such as sitting or sleeping.
Why Early Diagnosis is Crucial
Detecting psoriatic arthritis at an early stage can prevent irreversible joint damage and improve long-term outcomes. Timely interventions can halt disease progression and preserve joint function.
Diagnosis and Treatment
Diagnosis
A rheumatologist typically diagnoses psoriatic arthritis through a combination of physical examinations, patient history, and imaging tests such as X-rays or MRIs.
Treatment
Treatment generally involves medications like nonsteroidal anti-inflammatory drugs (NSAIDs), disease-modifying antirheumatic drugs (DMARDs), and sometimes biologics.
Frequently Asked Questions
Q: Can psoriatic arthritis occur without skin psoriasis?
A: Yes, psoriatic arthritis can occur independently, though it most commonly appears in individuals who already have skin psoriasis.
Q: Are there preventive measures for psoriatic arthritis?
A: While you can’t entirely prevent psoriatic arthritis, managing psoriasis symptoms and leading a healthy lifestyle can reduce the risks.
Q: Is psoriatic arthritis curable?
A: As of now, there is no cure for psoriatic arthritis, but treatments can manage symptoms and prevent joint damage.
Q: How quickly does the disease progress?
A: The speed of progression varies between individuals and depends on various factors such as age, overall health, and how promptly treatment is initiated.
Conclusion
Early diagnosis of psoriatic arthritis in the feet is essential for managing the condition effectively. Being aware of the visual signs like redness, swelling, and nail changes can be invaluable for timely intervention.